Top 9 Denial Appeal Platforms to Overturn More Denials and Recover Lost Revenue (2026 Guide)
Denial appeal platforms use AI to automate appeal drafting, prioritize high-value claims, and recover lost revenue while improving efficiency and reducing future denials.
April 27, 2026


Key Takeaways:
• Up to 60% of hospitals never appeal denials at all, adding up to roughly $3 million in lost revenue per year for a mid-sized 350-bed hospital (HFMA).
• A strong denial appeal platform should do three things well: AI-powered appeal drafting, root-cause analytics, and native EHR + RCM integration.
• Modern AI denial appeal platforms can draft payer-specific appeal letters, score each denial by recovery probability, and track filing deadlines automatically.
• Whether you keep appeals in-house or outsource them, the platform underneath your team is what determines how many appeals get worked, how fast, and at what quality.
Denial appeals sit at one of the most painful intersections in healthcare RCM.
They require clinical depth, payer-specific knowledge, tight deadline discipline, and high-volume execution. And most billing teams don't have those resources to spare.
So, they triage. They appeal the highest-dollar denials, let the smaller ones expire, and figure the lost revenue costs less than the labor to fight every claim. However, the math rarely works out.
As per HFMA, up to 60% of hospitals never appeal denials at all, adding up to roughly $3 million in lost revenue per year for a mid-sized 350-bed hospital. All of it walking out the door because no one had time to fight for it.
This is the gap that denial appeal platforms and services are built to close.
In this guide, we'll break down the top 9 denial appeal platforms and where each one fits best.
On this page
What Makes a Denial Appeals Solution Worth Using?
A denial appeal typically moves through three phases: detect and prioritize, build and review, submit and learn. What happens at each phase determines how much revenue actually gets recovered.
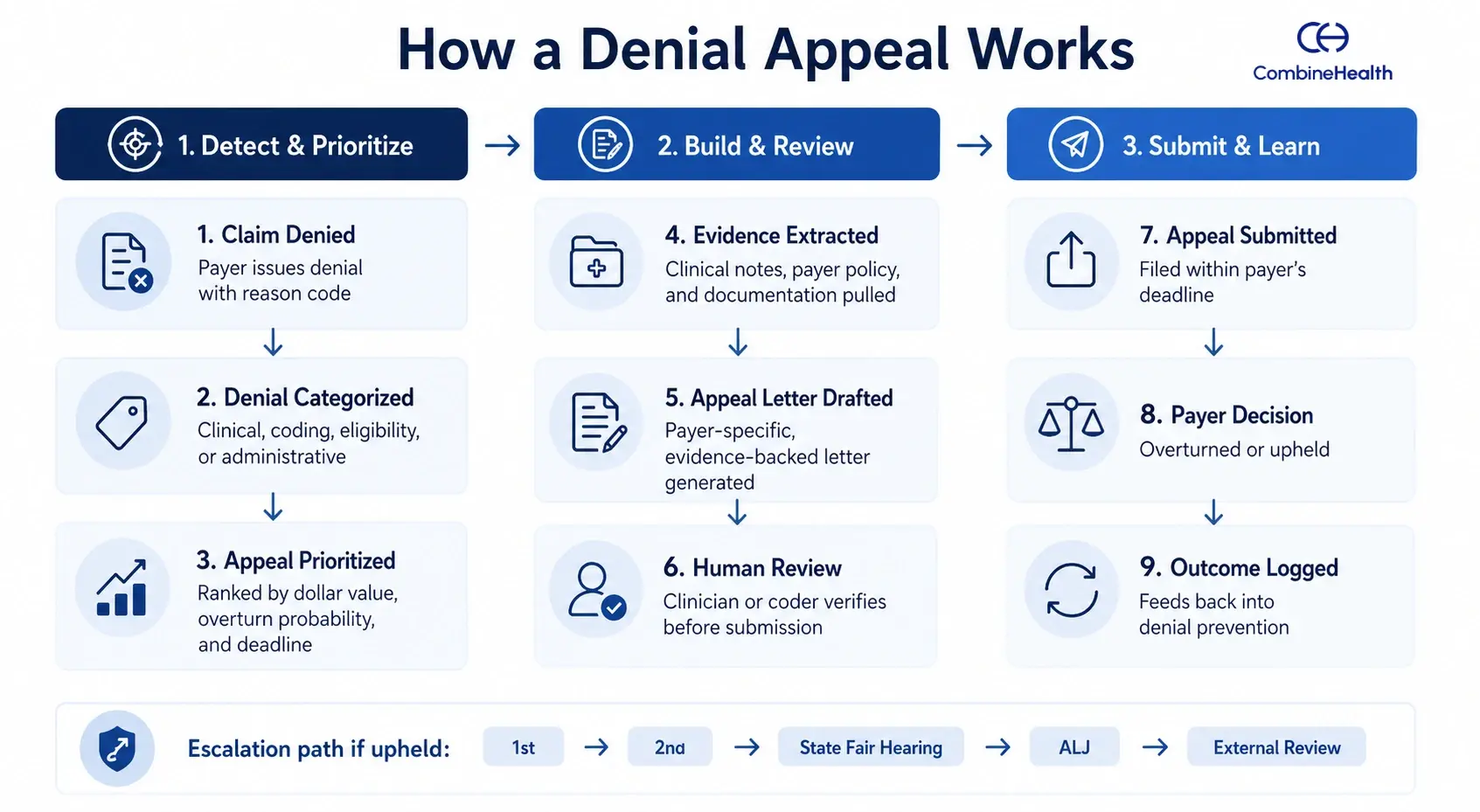
The denial appeal platform you choose should have these three core capabilities:
1. AI-powered Appeal Drafting
Writing the appeal letter is the biggest time sink in denial management. Strong solutions should generate payer-specific, evidence-backed letters automatically—pulling from clinical documentation and payer guidelines. Faster drafting means more appeals filed and more revenue recovered.
2. Root Cause Analytics
Recovering denied revenue matters. Preventing the next denial matters even more! A denial appeal platform should analyze denial patterns by payer, denial code, and provider to surface upstream systemic issues—so your team fixes the process gap as well, along with the claim.
3. EHR and RCM Integration
An appeal tool outside your existing workflow creates friction. Look for solutions that connect directly to your EHR, practice management system, and clearinghouse so data flows automatically.
Recommended reading: An Expert-Backed Playbook for Managing Claim Denials
Top 9 Denial Appeal Platforms in 2026
The vendors below span three categories—AI-native software, hybrid software-plus-services, and denial appeal services delivered by managed teams.
1. CombineHealth Rachel—AI-Native Appeal Platform
Rachel is CombineHealth's AI appeal solution—built to automate the slowest parts of the appeals workflow. Rather than assisting a human writing one appeal at a time, Rachel autonomously analyzes the denial, drafts a payer-specific medical necessity appeal, and prioritizes each case by recovery probability.
She reasons across documentation, payer policies, and historical outcomes the way a senior appeals specialist would and explains every decision in plain language so coders, auditors, and providers can verify the work.
Why Rachel Stands Out
- Evidence-based drafting: Pulls clinical documentation from the EHR, extracts the references that support medical necessity, and weaves them into payer-specific letters in minutes.
- Success probability scoring: Predicts the likelihood of overturn for each denial, so teams work the highest-yield appeals first.
- Deadline tracking: Monitors filing windows across every payer and appeal tier, with proactive reminders before cutoffs.
- Explainable AI with human-in-the-loop: Provides line-by-line rationale and flags low-confidence cases for human review.
Continuous learning: Every appeal outcome refines the model on which arguments work for which payers.
Recommended Reading: How to appeal a claim denial
Key Features:
- Drafts payer-specific appeal letters in minutes
- Adapts to your organization's writing style from prior successful appeals
- Custom denial rules per specialty or facility
- Integrates with existing EHR, PM, and billing systems
- Works with Adam (denial management solution) and Taylor (RCM analytics solution) for end-to-end coverage
- HIPAA-compliant with U.S. data residency
Best for: Mid-to-large hospitals, health systems, and multi-specialty groups that want to scale appeals volume without scaling labor—and need explainability auditors, and providers can trust.
Health Center Stops Revenue Leakage on 5,000 Claims a Month
CombineHealth delivered 97.4% accuracy across 10,000+ claims and a 20% reduction in denials, end-to-end.
Read the Case Study
2. OSP Labs
OSP Labs builds custom denial appeal management platforms rather than selling off-the-shelf software.
Their AI tools claim to reduce manual effort by up to 70% through automated letter generation, payer-specific rules engines, and real-time analytics dashboards.
The product also supports integration with EHR systems, which reduces the likelihood of manual data entry errors.
Key Features:
- Custom-built denial software per client requirements
- Payer rules engine that surfaces unpublished payer behavior
- Real-time analytics dashboard with win/loss ratio tracking
- EHR integration with automated appeal letter generation
Best for: Organizations that need a fully bespoke denial management system built around their specific workflows and EHR environment.
3. Savista RCM
Savista is a denial appeals services company with decades of experience, partnering with hundreds of hospitals and physician practices across the country.
Their clinical denial team handles medical necessity, level of care, DRG downgrades, and no-authorization denials.
Beyond working claims, they train physicians and PFS staff on denial prevention and deliver payer-specific reporting to address upstream root causes.
Key Features:
- Dedicated clinical denial team
- Physician and PFS staff training for upstream denial prevention
- Payer-specific reporting and root cause analysis
- Account evaluation, appeal creation, and follow-up
Best for: Healthcare organizations seeking a tenured outsourced partner for high-complexity clinical denials at scale.
4. HIS (Healthcare Information Services)
HIS specializes in orthopedic and radiology practices—settings where denial patterns and documentation requirements are highly specific.
With 30+ years of experience, their team reviews each denial and takes action within 24 hours, identifies root causes, and trends denial data by payer.
Their team also delivers direct feedback on documentation and coding improvements to reduce front-end errors over time.
Key Features:
- 24-hour action window on every denial
- Specialty-specific expertise in orthopedics and radiology
- Root cause identification and payer trend analysis
- Direct practice feedback on documentation and coding gaps
- Front-end process improvement recommendations
Best for: Orthopedic and radiology practices that need a denial management partner with deep specialty-specific expertise.
5. PayerWatch
PayerWatch is a denial and appeals vendor focused on clinical validation, medical necessity, and outpatient denials.
Its Veracity AI Appeal Engine drafts appeals in minutes with high claimed accuracy and every fact tied back to source documentation.
Veracity is EMR-agnostic and requires clinician verification before submission. AppealMasters, their clinical-legal team, handles escalations through ALJ hearings. Both are HITRUST CSF Certified.
Key Features:
- AI-Assisted Appeals with citation-grounded output
- Centralized denial, audit, and appeal workflow
- Clinical-legal services for ALJ hearings and external review
- EMR-agnostic integration (Epic, Cerner, MEDITECH)
- HITRUST CSF Certified
Best for: Hospitals and health systems needing defensible AI-assisted appeals with clinical-legal escalation support.
6. AnnexMed
AnnexMed offers denial appeal services as part of full-spectrum outsourced RCM, with extensive experience across more than 40 specialties and a strong client retention record.
The company covers 50+ specialties, including cardiology, ABA, home health, DME, and FQHC. The team consistently drives denial rates to low single digits and maintains a 24-48 hour turnaround on denied claims.
Their hybrid US and offshore team maintains HIPAA-compliant workflows while keeping operational costs accessible.
Key Features:
- 24-48 hour turnaround on denied claims
- Root cause analysis trended by payer
- Front-end claim corrections to prevent recurring denials
- Hybrid US and offshore staffing model
Best for: Mid-size physician groups, FQHCs, home health, DME, and specialty practices wanting offshore-leveraged denial outsourcing.
7. McBee Associates
McBee provides denial appeal services for complex, high-dollar appeals—medical necessity, DRG downgrades, and line-item denials.
Their team of registered nurses and certified coders brings deep clinical expertise to each case, with work spanning first, second, and third-level appeals, State Fair Hearings, and ALJ hearings.
They've recovered $74M over the past two years across named clients, including Texas Children's Hospital and Hackensack Meridian Health Network. McBee is part of Netsmart and AICPA SOC Certified.
Key Features:
- Full appeal escalation: 1st–3rd level, State Fair Hearings, ALJ
- RN and certified coder team with deep clinical expertise
- Proprietary analytics for documentation trend tracking
- Named health system clients with documented recovery outcomes
- AICPA SOC Certified
Best for: Hospitals and post-acute providers dealing with high-complexity clinical denials and regulatory audit responses.
8. Quadax
Quadax takes a workflow-first approach to denial management—intelligent routing, automated worklist creation, and escalation logic across the full denial lifecycle.
Quadax’s Decision Intelligence module runs real-time root cause analysis to improve clean claim rates.
Axis, their audit management tool, handles RAC and external audit responses. RemitMax, their remittance automation tool, converts paper EOBs to ANSI 835s automatically, keeping remittance data flowing into the denial workflow without manual intervention.
Key Features:
- ML-based Predictive Intelligence for pre-submission avoidance
- Automatic worklist creation with intelligent routing
- Appeal letter templates with auto-escalation logic
- Native Epic, Cerner, and MEDITECH integrations
Best for: Medical billing companies and multi-specialty groups managing high denial volumes that need structured workflow automation.
9. Datavant
Datavant's denial appeal platform is built on network reach. They have an embedded presence within the Health Information Management (HIM) function—the clinical records layer inside health systems.
That footprint spans the majority of the largest US health systems, giving them access to clinical and payer data that most denial vendors might not have.
That data advantage feeds denial prevention, retrospective analysis, defense audits, pre-certification support, and physician education—all grounded in documentation insight rather than workflow automation alone.
Key Features:
- Embedded HIM presence across the largest U.S. systems
- Automated appeal segmentation and generation
- Scalable staffing for pre-auth, appeal letters, and defense audits
Best for: Health systems already embedded in Datavant's network looking to turn their HIM infrastructure into a denial prevention advantage.
Why Every Denials Team Needs an AI-powered Denial Appeal Platform in 2026
Whether you keep denial work in-house or outsource it to a denial management services partner, the platform underneath your team is what determines how many appeals get worked, how fast, and at what quality.
An AI denial appeal platform changes the math for either setup:
- For in-house teams, it removes the bottleneck that forces triage in the first place. Appeals get drafted in minutes instead of hours, deadlines get tracked automatically, and your senior writers stop spending their day on routine cases.
- For outsourced teams, it turns the service from a labor-leveraged model into a tech-leveraged one. The same managed services partner can work 5-10x more appeals at a higher quality when an AI platform sits underneath their workflow.
So, whether you go with a denial appeals service or have an in-house team, a denial appeal platform underneath your team can help amplify their work. AI handles the routine, high-volume appeals, while humans escalate the complex clinical and legal cases.
How To Choose the Right Denial Appeal Platform?
The right platform closes the specific gaps costing your organization recoverable revenue. Below are the capabilities to evaluate when comparing denial appeal platforms and denial appeal services.
1. Clinical Appeal-Letter Quality
Overturn rates rise and fall with letter quality. Look for platforms that draft letters tailored to each payer's review process and not generic templates.
Recommended resource: Sample denial appeals letter
2. Payer-Specific Policy Logic
Strong platforms apply payer-specific LCDs, NCDs, contract language, and modifier rules to every appeal and update those rules as policies evolve.
3. Deadline and Escalation Management
Filing windows vary by payer, reason, and appeal level. The right platform monitors every deadline and escalates proactively.
4. Explainability and Human-in-the-Loop
Appeals that escalate to the Administrative Law Judge (ALJ) hearing (the third level of Medicare's appeals process) or external review need an audit trail. The best AI denial management platforms show a line-by-line rationale for every recommendation.
5. Integration with Your Stack
Look for denial appeal platforms that integrate natively with your EHR, PM, and clearinghouse, without heavy IT involvement.
6. Continuous Learning
The best platforms get smarter over time, refining which arguments work for which payers and denial reasons.
Automate Your Denial Appeals End-to-End
If you're ready to put that platform layer in place, CombineHealth's Rachel was built for this exact play—an AI appeals platform that amplifies whatever team setup you already have.
Rachel handles the entire appeals workflow (evidence extraction, payer-specific drafting, deadline tracking, and continuous learning) in one connected system.
Paired with Adam (denial management solution) and Taylor (RCM analytics solution), Rachel feeds outcomes back into upstream RCM to prevent the same denial pattern from recurring.
Book a demo with us to see how Rachel can turn unappealed denials into recovered revenue without adding a single hire to your team!
FAQs
1. What is a denial appeal platform?
A denial appeal platform is software that automates how healthcare organizations identify, draft, submit, and track appeals for denied insurance claims. Modern platforms use AI to extract clinical evidence, generate payer-specific appeal letters, prioritize denials by recovery probability, and track filing deadlines.
2. What's the difference between denial management and denial appeals?
Denial management is the broader umbrella—preventing, tracking, and resolving denied claims, including correcting and resubmitting them. Denial appeals are a specific subset focused on formally challenging a payer's denial decision through written appeals, supporting documentation, and (when needed) escalation to ALJ hearings or external review.
3. Can AI write medical appeal letters?
Yes, but the best denial appeal platform should keep humans in the loop. AI handles the drafting (pulling clinical evidence from the EHR, applying payer-specific policy logic, structuring the medical necessity argument), and clinicians or coders verify before submission.
Recommended Reads
Related Posts
Lorem ipsum dolor sit amet, consectetur adipiscing elit. Suspendisse varius enim in eros elementum tristique. Duis cursus, mi quis viverra ornare, eros dolor interdum nulla, ut commodo diam libero vitae erat. Aenean faucibus nibh et justo cursus id rutrum lorem imperdiet. Nunc ut sem vitae risus tristique posuere.
Subscribe to newsletter - The RCM Pulse
Trusted by 200+ experts. Subscribe for curated AI and RCM insights delivered to your inbox
Let’s work together and help you get paid
Book a call with our experts and we'll show you exactly how our AI works and what ROI you can expect in your revenue cycle.
Email: info@combinehealth.ai
















