Top 10 AI Denial Management Solutions for Reducing Healthcare Revenue Leakage in 2026
Explore our compilation of the top 10 denial management solutions for healthcare RCM teams in 2026 and understand the standout features that makes them worth your investment.
February 23, 2026
.webp)

Key Takeaways:
• Denials are rising, with an 11.65% initial denial rate, hospitals are losing revenue on more than 1 in 9 claims. Manual follow-up alone can’t keep up with payer complexity and staffing shortages.
• Modern denial management platforms predict high-risk claims, auto-generate appeals, and uncover root causes to prevent repeat denials.
• The best AI denial management solutions combine prevention, automation, and analytics. End-to-end tracking, predictive scoring, and intelligent prioritization are now table stakes.
• Different healthcare denial management tools serve different needs. Some focus on autonomous AI (CombineHealth), others on analytics (MedEvolve), appeals automation (Waystar), voice AI (Kyron), or hybrid services (Optum, Datavant).
• To measure the ROI of a denial management software, organizations should track clean-claim rate (>90%), denial rate (<5%), and overturn rate (>65%) to ensure real revenue impact.
Healthcare claim denials are no longer occasional disruptions, but a frequent occurrence.
In 2025, the average initial denial rate stands at 11.65%, meaning more than one in every nine claims is rejected on first submission.
What makes it even more challenging is that payer rules change frequently and staffing shortages limit how quickly teams can respond. Plus, manual follow-up simply doesn’t scale.
AI-powered denial management solution are helping streamline this process and get hospitals paid faster.
In this guide, we break down the Top 10 AI denial management solutions for healthcare RCM teams to protect their net revenue in 2026.
On this page
- How Does a Healthcare Denial Management Software Work?
- How Can Healthcare Denial Management Services Improve Revenue Cycle Efficiency?
- 10 Best AI Denial Management Solutions in 2026
- 1. CombineHealth: AI-Powered End-to-End Denial Management Software
- 2. MedEvolve
- 3. Waystar’s Denial and Appeals Automation
- 4. Experian Denial Management
- 5. Kyron Medical
- 6. Rivet Claims Resolution
- 7. Finthrive Fusion
- 8. Optum A/R Recovery and Denial Management
- 9. SmarterDx SmarterDenials
- 10. Datavant Denial Management
- How To Choose a Healthcare Denial Management Software
- How to Measure the Success of a Denial Management Service?
- Ready to Move From Reactive Denial Cleanup to Proactive Revenue Protection?
- FAQs
- What is Denial Management in Healthcare RCM?
- Which Companies Specialize in Healthcare Denial Management in the USA?
- What Are the Top 10 Denials in Medical Billing?
- What Are the Different Types of Claims Denial Appeals in Healthcare?
- How Can I Effectively Reduce Claim Denials in Medical Billing?
- What Features Should I Look for in Healthcare Denial Management Solutions?
How Does a Healthcare Denial Management Software Work?
A healthcare denial management software typically operates across the full denial lifecycle, which includes these stages:
1. Denial Categorization
When remittance files return with denials, the platform:
- Reads CARC/RARC codes and payer messages
- Normalizes denial reasons across payers
- Groups them into actionable categories (e.g., eligibility, coding, authorization, medical necessity)
2. Intelligent Routing and Resolution
Denied claims are routed into prioritized worklists based on:
- Dollar value
- Filing deadlines
- Payer behavior
- Likelihood of overturn
Staff receive contextual support, such as required documentation, prior similar cases, and suggested corrections. Many systems pre-populate corrected claims, auto-draft appeal letters, and track resubmissions through final resolution.
3. Denial Dashboards
Dashboards monitor denial rates, recovery rates, and days-to-appeal. Insights are fed back to registration, coding, and documentation teams—closing the loop and reducing repeat denials over time.
.webp)
How Can Healthcare Denial Management Services Improve Revenue Cycle Efficiency?
Healthcare denial management services improve efficiency by reducing preventable claim denials, accelerating recovery, and turning denial data into operational improvements across the revenue cycle. Here’s what it offers:
Faster Cash Flow and Lower A/R Days
Structured denial follow-up with defined timelines, escalation rules, and consistent reporting keeps claims from aging out.
Higher Clean-Claim Rates
Tech-enabled services apply payer logic, documentation checks, and denial trend analysis before and after submission.
- Root causes are identified by payer, code, specialty, or location
- Upstream fixes reduce repeat denials and rework
- Many organizations see measurable drops in denial rates after implementing structured workflows
Lower Cost-to-Collect
Reworking a denial can cost tens of dollars per claim. Preventing and resolving them efficiently reduces administrative waste.
- Automated tracking and alerts reduce manual touchpoints
- Standardized processes eliminate duplication
- Specialized teams focus on high-impact recovery work
Improved Net Revenue
Effective hospital denial management strategies recover revenue that would otherwise be written off. AI-driven validation and predictive risk scoring improve clean-claim performance, while structured appeals increase overturn rates.
10 Best AI Denial Management Solutions in 2026
1. CombineHealth: AI-Powered End-to-End Denial Management Software
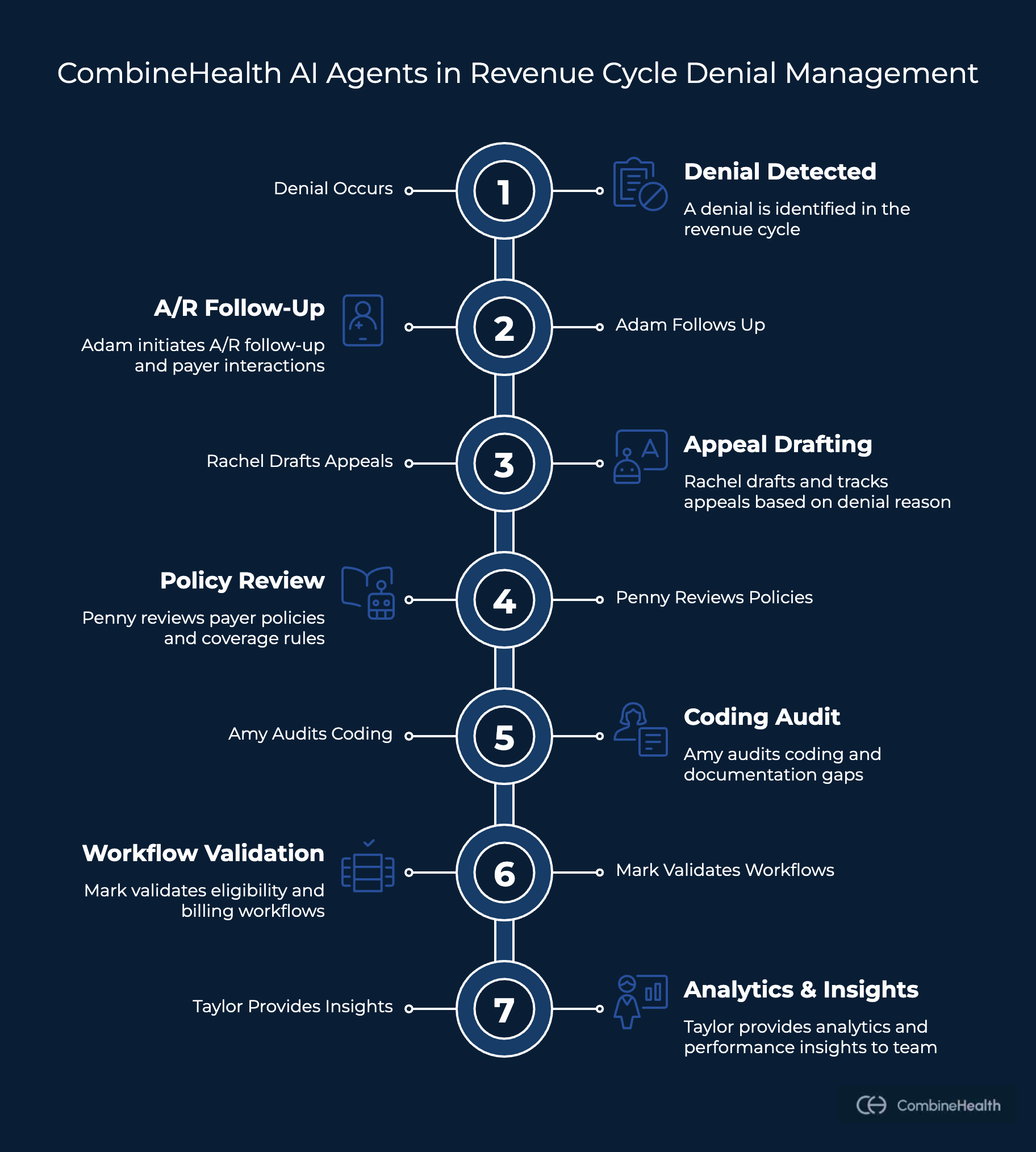
CombineHealth’s Denial Management Suite takes a comprehensive approach to both preventing and resolving denials. Instead of treating denial management as a back-end clean-up function, CombineHealth connects multiple AI agents that work together across the revenue cycle, whenever a denial shows up. Here’s how:
- Adam manages A/R follow-up and payer interactions
- Rachel drafts and tracks appeals
- Penny reviews payer policies and coverage rules
- Amy audits coding and documentation gaps
- Mark validates eligibility and billing workflows
- Taylor provides analytics and performance insights
Now, what makes these AI agents stand out is their ability to sync up during the denial management workflow. For example, Adam can consult Penny for policy clarification, pull coding validation from Amy, or trigger Rachel to generate a payer-specific appeal — creating a tightly integrated denial response engine.
Beyond handling denials as they occur, CombineHealth’s denial management suite also proactively reduces future denials by identifying:
- Documentation deficiencies
- Coding inconsistencies
- Authorization risks
- Payer-rule conflicts
And all this is done before the claims are submitted.
Key Features
- Autonomous AI agents: Coordinated bots handle prevention, appeals, and follow-up end-to-end.
- Proactive denial prevention: Flags documentation, coding, and eligibility gaps before submission.
- AI-generated appeals: Drafts payer-specific letters and manages resubmissions automatically.
- Smart prioritization: Focuses teams on high-value, high-probability recoveries.
- Continuous denial intelligence: Identifies root causes to reduce repeat denials.
Best for: Large hospitals and health systems looking to scale denial management operations without adding headcount.
2. MedEvolve
MedEvolve addresses denial management through its Effective Intelligence (Ei) platform, combining real-time analytics, workforce automation, and generative AI.
Instead of focusing only on resolving denials after they occur, the denial management platform measures every human touch on a claim, identifies avoidable work, and helps organizations reduce preventable denials by optimizing workflows across the revenue cycle.
Key Features
- Effective Intelligence (Ei) analytics: Tracks zero-touch rate, denial-related touches, and staff productivity.
- Touch reduction automation: Routes staff away from low-value work and toward high-risk claims.
- Generative AI insights: Detects shifts in denial trends and explains underlying drivers.
- End-to-end visibility: Connects front-end, mid-cycle, and back-end processes to pinpoint root causes.
- Embedded RCM optimization: Integrates analytics into daily workflows to continuously reduce denials and labor dependency.
Best For: Mid- to large-size provider groups and RCM organizations aiming to reduce manual workload.
3. Waystar’s Denial and Appeals Automation
Waystar’s Denial + Appeal Management platform combines predictive analytics, generative AI, and automation to help providers overturn denials faster and prevent repeat issues.
Designed for high-volume environments, it prioritizes the most valuable denials, auto-generates payer-specific appeals, and integrates with enterprise systems to streamline resolution at scale.
Key Features
- Predictive prioritization: Scores and routes denials based on the likelihood of overturn and financial impact.
- Generative AI appeals: Drafts payer-specific letters using an extensive template library.
- Paperless workflows: Supports batch submissions, proof-of-delivery tracking, and exception handling.
- Auto Coverage Detection: Verifies updated eligibility data for coverage-related denials.
- Advanced denial analytics: Identifies root causes and trends to reduce future denials.
Best for: Large health systems and multispecialty providers managing high denial volumes.
4. Experian Denial Management
Experian Health’s Denial Workflow Manager, enhanced by AI Advantage, automates the detection, prioritization, and resolution of denied, held, suspended, and zero-pay claims.
By leveraging ERA/ECS data, predictive analytics, and integrated workflows, the platform standardizes follow-up, eliminates manual remittance review, and provides actionable root-cause insights to improve clean-claim performance.
Key Features
- Automated denial detection: Identifies denials, holds, zero pays, and appeal outcomes directly from ERA/ECS data.
- Customizable worklists: Prioritizes follow-up by denial type, dollar value, and organizational rules.
- Root-cause analytics: Tracks denial trends by payer, procedure, and department to prevent recurrence.
- AI Advantage™ tools: Predicts high-risk claims pre-submission and triages appeals by overturn probability.
- ClaimSource integration: Unifies claims and denials data for corrections and resubmissions in one view.
Best for: Mid- to enterprise-level providers seeking integrated, AI-driven workflows to automate denial follow-up and accelerate cash flow.
5. Kyron Medical
Kyron Medical is an AI-native platform that deploys voice AI agents to handle denial follow-up, claim status checks, eligibility verification, and prior authorizations by calling payers directly. It automates phone-based interactions, posts structured notes back into a centralized dashboard, and integrates with EHRs and clearinghouses to reduce manual workload and accelerate resolution.
Key Features:
- AI voice agents: Calls payers, navigates IVRs, conducts conversations, and logs outcomes with a full audit trail.
- Automated claim status checks: Retrieves updates on denied or pending claims and posts structured notes in real time.
- Centralized dashboard: Monitor AI performance and manage denial, eligibility, and auth workflows in one place.
- Seamless integrations: Connects with EHRs, clearinghouses, payer portals, and ERP systems.
- Ongoing optimization: Continuous model tuning and support to improve overturn rates and cycle times.
Best for: Mid-size RCM teams looking to eliminate payer hold times and automate voice-based denial follow-up without heavy IT investment.
6. Rivet Claims Resolution
Rivet is a denial management platform purpose-built for resolution efficiency. Designed as a hands-on workhorse for billing teams, it combines customizable worklists, batch processing, and automation to streamline appeals and maximize revenue recovery—without percentage-based collections fees.
Key Features
- Customizable worklists: Flexible filtering and batch workflows to prioritize and process denials efficiently.
- Automated denial analysis: Identifies root causes, predicts revenue impact, and applies billing edits to prevent repeat issues.
- Workflow documentation: Captures expert handling steps and attaches them to similar denials for consistency.
- On-demand analytics: Instant custom reports on denial trends, payer behavior, and recovery performance.
- Revenue recovery tools: Supports bulk resubmissions and audits for underpayments without contingency fees.
Best for: Small to mid-size practices, billing companies, and lean RCM teams.
7. Finthrive Fusion
FinThrive Fusion is an AI-driven data and intelligence layer embedded across the FinThrive RCM platform. Rather than functioning as a standalone denial tool, Fusion connects EHRs, billing systems, and payer data into a unified fabric that powers predictive models and dynamic workflows. The result: a shift from reactive denial clean-up to proactive, enterprise-wide revenue optimization.
Key Features
- Dynamic denial prevention workflows: Learns from payer behavior and adapts processes to reduce future denials.
- AI-powered analytics: Surfaces billing errors, denial trends, and revenue leakage in near real time.
- Cross-cycle intelligence: Shares denial insights across authorization, claims, pricing, and collections.
- Denials & Underpayments Analyzer: Identifies underpayments and denial risks as part of enterprise performance management.
- Agentic AI workflows: Automates high-volume, rules-based revenue tasks tied to denial intervention.
Best for: Large hospitals and health systems leveraging the FinThrive ecosystem.
8. Optum A/R Recovery and Denial Management
Optum’s A/R Recovery and Denial Management solution combines managed services with enabling technology to reduce denials and accelerate cash recovery.
Instead of offering a standalone software tool, Optum embeds recovery specialists into existing workflows and supports them with analytics, automation, and reporting to resolve backlogs, address aged A/R, and strengthen denial performance over time.
Key Features
- Dedicated recovery teams: HFMA-certified specialists work denial backlogs, trend denials, and underpayments within your current processes.
- Automated claim workflows: Classifies claims and guides structured follow-up with actionable intelligence.
- Root-cause analytics: Identifies systemic drivers of denials to support prevention strategies.
- Configurable technology layer: Provides reporting and performance visibility tied to recovery outcomes.
- Flexible engagement models: Project-based, supplemental, or ongoing support without permanent headcount increases.
Best for: Hospitals and health systems with aged A/R, recurring denial trends, or staffing gaps.
9. SmarterDx SmarterDenials
SmarterDenials is a clinical AI platform designed to automate evidence-backed appeal letters for denied claims. By analyzing payer denial reasons against full patient records, (including notes, labs, and coding) it generates comprehensive appeals in minutes, reducing manual chart review time for complex clinical denials while keeping teams in control of final submissions.
Key Features
- Clinical denial analysis: Identifies discrepancies between payer rationale and documented care.
- Evidence extraction: Pulls structured and unstructured data from charts, scans, and faxed EOBs.
- Generative AI appeals: Produces payer-ready letters with clinical evidence and coding references.
- Human review workflow: Allows teams to edit and approve appeals before submission.
- Focused on complex denials: Optimized for DRG downgrades, level-of-service, and medical necessity cases.
Best for: Hospitals managing high volumes of clinical denials who need faster, evidence-driven appeals.
10. Datavant Denial Management
Datavant delivers a hybrid denial management model that blends technology, specialized staffing, and clinical expertise.
The solution addresses current denials while implementing systemic fixes to prevent future ones — combining automated appeals, scalable recovery teams, and documentation improvement strategies to reduce revenue leakage across inpatient and outpatient workflows.
Key Features
- Automated appeals: Segments denials, predicts overturn likelihood, and generates ready-to-send appeal letters.
- Scalable staffing support: Provides short- and long-term experts for pre-auths, appeals, audits, and revenue integrity.
- Denial prevention programs: Identifies documentation and coding gaps to eliminate systemic avoidable denials.
- Clinical education & expertise: Offers physician training and utilization review guidance to strengthen compliance.
- RCM system integration: Works within existing workflows to recover high-dollar claims and improve revenue accuracy.
Best for: Health systems seeking a combined technology and staffing approach to manage complex, high-volume denials.
How To Choose a Healthcare Denial Management Software
Here’s what you should look for in a healthcare denial management software:
Core Denial Management Capabilities
Look for denial management solutions with strong operational fundamentals, such as:
- End-to-end tracking: Centralized view of denied claims, codes, notes, and outcomes
- Pre-submission rules engine: Configurable payer edits, eligibility, and prior auth checks
- Smart worklists: Auto-assignment, SLA timers, escalation rules
- Integrated denials and appeals management: Templates, document checklists, and resolution tracking
- Deep system integration: Seamless EHR, PM, clearinghouse, and remit connectivity
Analytics and Root-Cause Intelligence
Look for solutions that go beyond surface-level reporting.
- Denial dashboards by payer, provider, specialty, and financial impact
- Normalized CARC/RARC mapping to uncover true root causes
- Predictive scoring for in-flight claims
- Clear reporting on A/R reduction, write-off avoidance, and cash lift
Automation, Scalability, and Security
Finally, assess usability and enterprise readiness:
- RPA for payer portal tasks and status checks
- Real-time deadline alerts
- Role-based dashboards
- HIPAA-compliant architecture with audit trails
How to Measure the Success of a Denial Management Service?
To measure the success of a denial management service, organizations typically monitor these three metrics:
Ready to Move From Reactive Denial Cleanup to Proactive Revenue Protection?
The denial management platforms in this list show how AI is reshaping denial management. But the biggest impact comes from connecting prevention, appeals, follow-up, and analytics into one coordinated system.
If you're ready to move from reactive denial cleanup to proactive revenue protection, book a demo with CombineHealth and see how autonomous AI agents can reduce denials and accelerate cash flow at scale.
FAQs
What is Denial Management in Healthcare RCM?
Denial management in healthcare revenue cycle management (RCM) is the process of identifying, analyzing, appealing, and preventing insurance claim denials. It involves tracking denial reasons, correcting errors, resubmitting claims, and addressing root causes to improve clean-claim rates, reduce A/R days, and protect net revenue.
Which Companies Specialize in Healthcare Denial Management in the USA?
Several companies specialize in denial management, including CombineHealth, Waystar, Experian Health, MedEvolve, FinThrive, Optum, Datavant, SmarterDx (SmarterDenials), Rivet, and Kyron Medical. These vendors offer combinations of AI-driven software, automation, analytics, and managed services to prevent denials and accelerate recovery.
What Are the Top 10 Denials in Medical Billing?
Common denial categories include eligibility issues, missing prior authorization, coding errors, medical necessity denials, duplicate claims, incorrect patient information, bundling/NCCI edits, timely filing limits, modifier errors, and coordination of benefits (COB) issues. Many of these are preventable with stronger front-end validation and payer rule checks.
What Are the Different Types of Claims Denial Appeals in Healthcare?
The two main types of appeals are internal appeals and external reviews.
An internal appeal is the first step, where the insurer re-evaluates the denial, sometimes through an expedited review. If unsuccessful, an external review involves an independent third party assessing the claim, often for medical necessity disputes.
How Can I Effectively Reduce Claim Denials in Medical Billing?
Effective denial reduction includes strengthening eligibility verification, prior authorization checks, coding accuracy, and documentation completeness before submission. Ongoing denial analytics, root-cause analysis, staff training, and AI-powered predictive validation further improve clean-claim rates and reduce repeat denials.
What Features Should I Look for in Healthcare Denial Management Solutions?
In a healthcare denial management solution, look for features like:
- End-to-end denial tracking
- Payer rule engines
- Predictive analytics
- AI-generated appeals
- Smart prioritization
- Seamless EHR integration
- Strong denial analytics capabilities
Solutions should also offer explainable AI, automation for follow-up tasks, and measurable impact on A/R reduction and net collections.
Recommended Reads
Related Posts
Lorem ipsum dolor sit amet, consectetur adipiscing elit. Suspendisse varius enim in eros elementum tristique. Duis cursus, mi quis viverra ornare, eros dolor interdum nulla, ut commodo diam libero vitae erat. Aenean faucibus nibh et justo cursus id rutrum lorem imperdiet. Nunc ut sem vitae risus tristique posuere.
Subscribe to newsletter - The RCM Pulse
Trusted by 200+ experts. Subscribe for curated AI and RCM insights delivered to your inbox
Let’s work together and help you get paid
Book a call with our experts and we'll show you exactly how our AI works and what ROI you can expect in your revenue cycle.
Email: info@combinehealth.ai
.webp)















