Top 10 AI Healthcare Billing Software for Hospitals to Cut Denials and Accelerate Cash Flow (2026 Guide)
Explore our compilation of the top 10 AI medical billing solutions that can help you process claims faster and reduce denials.
May 19, 2026


Key takeaways:
• Medical billing demands more from billing teams than any other stage of the revenue cycle—medical billing solutions are helping health systems reduce errors, accelerate reimbursements, and bring denial rates under control.
• Not all medical billing software is built the same—some automate one workflow while others cover the full billing cycle end to end.
• The best medical billing solution for your organization depends on your claim volume, payer mix, EHR stack, and how much of the billing cycle you need automated.
• When evaluating any medical billing solution, prioritize end-to-end automation, native EHR integration, payer-specific billing logic, and proactive denial prevention.
Medical billing remains one of the most labor-intensive and error-prone stages of the healthcare revenue cycle.
Billing teams are stretched to their limits between constantly changing payer rules, manual charge entry, and the back-and-forth of claim follow-ups. When teams are this overloaded, errors become inevitable—and every error that slips through increases the likelihood of a denial.
Each denial then triggers a rework cycle that costs time, labor, and money to resolve—and those costs add up faster than most organizations realize. According to HFMA, reworking a single Medicare Advantage denial costs $47.77 on average, while commercial denials run $63.76 each. Multiply that by the denials a healthcare organization faces each month, and the numbers climb fast.
This additional rework directly delays reimbursements, stretches days in A/R, and quietly erodes the margins that health systems are already fighting to protect.
This is one of the biggest reasons healthcare organizations are turning to AI solutions to reduce billing errors, streamline claim submissions, accelerate reimbursements, and bring denial rates under control.
In this guide, we break down the top 10 AI medical billing solutions, explaining their features, automation depth, integrations, and pricing.
On this page
- What Is AI Medical Billing Software?
- Why AI Is Important in a Medical Billing Solution
- How Medical Billing Solutions Help Reduce Claim Denials and Accelerate Revenue
- What to Look for in a Medical Billing Software in 2026
- Top 10 AI Medical Billing Solutions for 2026
- How Hospitals Should Evaluate Medical Billing Platforms
- Automate Your Medical Billing End-to-End
- FAQs
What Is AI Medical Billing Software?
AI medical billing software uses artificial intelligence to automate and optimize healthcare revenue cycle workflows such as medical coding, claims submission, denial prevention, payment posting, and reimbursement management.
Unlike traditional billing systems that rely heavily on manual review and reactive workflows, AI-powered billing platforms analyze claims data in real time to identify coding errors, predict denials before submission, prioritize high-risk accounts, and accelerate reimbursements.
Why AI Is Important in a Medical Billing Solution
AI compresses hours of manual billing work into minutes, while reducing the errors that come with doing it by hand.
- It automates repetitive, rules-driven tasks. Eligibility verification, charge entry, payment posting, and claim status checks follow predictable logic. AI handles these autonomously, freeing billing staff to focus on exceptions and judgment calls.
- It creates a tighter feedback loop that reduces errors over time. AI flags CDI gaps, identifies coding inconsistencies, and surfaces patterns from prior denials—catching errors pre-submission rather than post-rejection.
- It speeds up claim processing dramatically. Tasks that take billing teams hours (or days) can be completed in minutes, from verifying eligibility across payer portals to scrubbing and submitting claims.
AI medical billing solutions are increasingly being utilized to mitigate these challenges, and this shift is happening across the industry. According to a McKinsey survey, 85% of healthcare leaders are already exploring or adopting generative AI, and among those implementing it, 64% report positive ROI.
Medical billing is one of the areas seeing the fastest adoption, because the workflows are repetitive, rules-driven, and high-volume—exactly where AI delivers the most impact.
How Medical Billing Solutions Help Reduce Claim Denials and Accelerate Revenue

AI medical billing solutions improve revenue cycle performance by tackling the root causes of delayed reimbursements, claim denials, and revenue leakage:
1. Fewer eligibility-related denials: AI verifies patient coverage across payer portals before services are rendered, catching issues that would otherwise result in rejected claims.
2. Higher clean claim rates: Automated validation of codes, modifiers, and payor-specific SOPs means claims go out right the first time.
3. Eliminated manual data entry errors: Charges are prepared and entered directly into billing software without manual workflows, which leads to mistakes.
4. Faster reimbursement cycles: Claims are scrubbed, submitted, and tracked electronically, reducing days in A/R.
5. Smarter denial prevention over time: Adopting an AI-powered medical billing software could identify patterns from historical data and adjust billing behavior to prevent repeat issues.
Recommended reading: AR scenarios in healthcare
What to Look for in a Medical Billing Software in 2026
Each step in medical billing comes with its own payer-specific rules and edge cases. Traditional medical billing software handles these steps in isolation, requiring billing staff to manually bridge the gaps between systems and workflows.
In 2026, the most important shift to look for is agentic AI—where multiple, role-specific AI agents work together like employees toward a shared goal: getting claims paid accurately and on time.
Unlike traditional automation that follows scripted rules, agentic AI systems can:
- Navigate 50+ payer portals autonomously to verify eligibility and benefits in real time.
- Read ERAs and EOBs—including scanned PDFs—to reconcile payments without manual intervention.
- Generate superbills by pulling encounter data, applying payer-specific coding rules, and preparing charges for submission.
- Learn continuously from outcomes and feedback to reduce repeat denials
Top 10 AI Medical Billing Solutions for 2026
1. Mark by CombineHealth—Best AI Medical Billing Solution by 2026’ Standards
CombineHealth's Mark is the most comprehensive AI medical billing solution in the U.S. market for 2026. Mark handles billing end-to-end by integrating directly into existing EHR and practice management workflows, navigating payer portals autonomously, and applying payor-specific billing SOPs to every claim.
Why Mark Stands Out
What sets Mark apart from every other tool on this list is its scope. While most solutions solve one piece of the billing puzzle, Mark covers eligibility through reconciliation in a single connected workflow—and gets smarter with every claim cycle by learning from prior denial patterns.
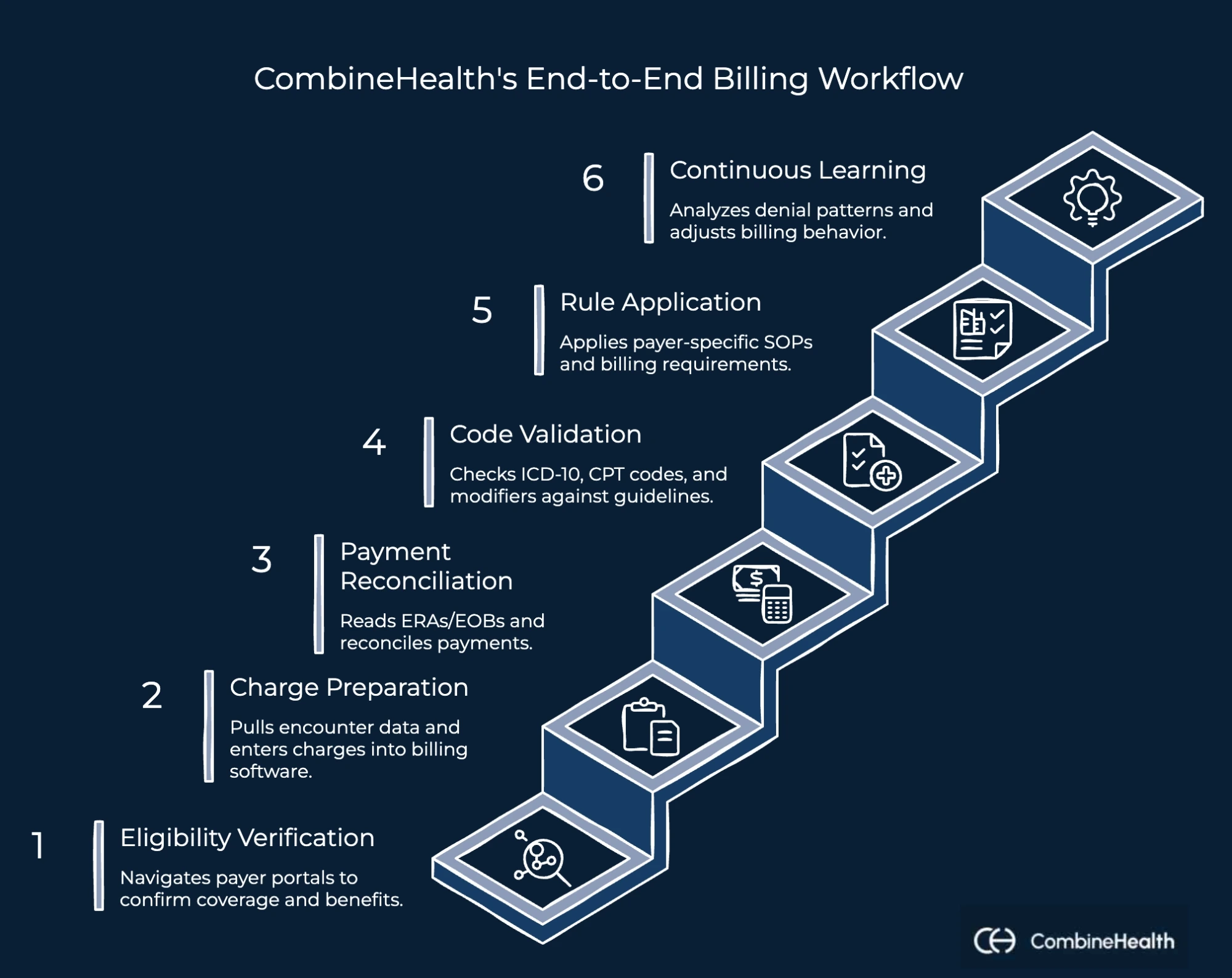
- Eligibility verification: Navigates 50+ payer portals and aggregators to verify patient coverage and benefits before services are rendered.
- Code and modifier validation: Checks diagnosis and procedure codes against payer-specific guidelines to catch errors before submission.
- Payer-specific rule application: Applies each payer's unique SOPs, modifier rules, and billing requirements to every claim.
- Charge preparation and superbill generation: Pulls encounter data, prepares charges, and enters them directly into billing software—eliminating manual data entry.
- Payment reconciliation: Reads ERAs and EOBs, including scanned PDF EOBs, to post payments and reconcile totals automatically.
- Continuous learning: Analyzes prior denial patterns and adjusts billing behavior to prevent repeat issues with every claim cycle.
Key Features
- Processes hundreds of claims in minutes
- Handles billing end-to-end by integrating seamlessly with existing EHR/PM workflows
- Seamlessly navigates 50+ payer portals and aggregators to perform patient eligibility checks
- Human-in-the-loop workflows for complex billing scenarios
- Enterprise-grade security with SOC 2 and HIPAA compliance; US data residency
Best for: Mid-to-large health systems, multi-specialty groups, and high-volume practices that want a single AI agent handling the full billing cycle without adding headcount or replacing existing systems.
2. Stedi
Stedi (commonly known as Stedi Claims) is the only API-first, programmable healthcare clearinghouse in the market.
Rather than offering a traditional billing UI, Stedi provides JSON-native APIs that let developer teams build custom billing workflows on top of modern clearinghouse infrastructure.
Stedi connects to multiple U.S. payers and supports all major HIPAA X12 transaction types, including eligibility, claims, claim status, and ERAs. Its pricing is fully transparent and pay-as-you-go.
Key Features
- RESTful, JSON-native APIs for claims, eligibility, ERA, and claim status
- Automated claim edits covering all SNIP types
- Built-in payer redundancy with automatic failover routing
- MCP server enabling AI agents to interact with clearinghouse functions programmatically
- Transparent, pay-as-you-go pricing with a free tier available
Best For: Health tech companies and developer teams building custom AI-powered billing platforms on top of programmable clearinghouse infrastructure.
3. EZClaim
EZClaim is one of the most affordable and straightforward medical billing solutions on the market.
It is ideal for solo providers, small practices, and billing companies that want reliability and ease of use without enterprise complexity.
EZClaim integrates with multiple clearinghouses and gives billing teams the flexibility to route claims through their preferred partner rather than locking them into a single clearinghouse.
Key Features
- Multi-clearinghouse support connecting to a wide range of payers
- Transparent per-user pricing with no contracts
- Responsive US-based customer support
- Customizable financial reporting
- Intuitive interface designed for small billing operations
Best for: Solo providers, small practices, and budget-conscious billing companies.
4. Prosper AI
Prosper AI, instead of processing claims through software workflows, deploys voice AI agents that pick up the phone and call payers directly.
It handles claim follow-ups, EOB retrieval, prior authorization, and eligibility verification the same way a human billing rep would, but at scale.
For RCM companies and offshore BPOs where phone-based payer work is a core cost driver, it converts what was previously a hard-to-scale labor function into an automated, measurable workflow.
Key Features
- Voice AI agents that call payers directly for claim follow-up, denial information, and EOB retrieval
- Automated prior authorization initiation and follow-up
- Real-time eligibility and benefits verification via voice
- Pre-built "Blueprints" for common healthcare call workflows
- HIPAA compliant with BAA, SOC 2 Type II certified, end-to-end encryption
- Integrates with EHR/PM systems and supports Zapier for custom workflows
Best for: Health organizations, specialty groups, and billing companies looking to automate phone-heavy payer workflows.
5. Anatomy
Anatomy Financial focuses on a specific but costly problem: converting paper-based insurance payments into structured electronic data.
Its AI converts paper and PDF EOBs into standardized 835 ERA files automatically, while Smart Reconciliation matches remittances against bank deposits without manual intervention.
If your organization is still manually processing paper EOBs and physical checks, Anatomy could be your solution to eliminate that bottleneck.
Key Features:
- AI-powered conversion of paper EOBs to electronic 835 remittance files
- Automated bank reconciliation between payer payments and deposits
- AI lockbox service for digitizing physical mail and check processing
- SOC 2 and HIPAA compliant
Best for: Practices, billing companies, and dental organizations processing high volumes of paper-based payments that need to automate payment posting and reconciliation.
6. Trizetto Provider Solutions
Trizetto, owned by Cognizant, is one of the largest enterprise healthcare clearinghouses in the United States.
They also provide an RCM platform that offers a comprehensive feature set, including claims scrubbing, ERA/EOB conversion, real-time eligibility, prior authorization, denial management, and contract compliance auditing.
Trizetto is built for large-scale operations that need enterprise-grade clearinghouse infrastructure with deep payer connectivity and ML-powered claim editing.
Key Features:
- ML-powered Advanced Claim Editing for proactive denial prediction
- Broad payer connectivity and direct EMR integrations
- Prior authorization with Da Vinci-compliant FHIR APIs
- Denial management with automated appeals
- Emerging agentic AI framework from Cognizant
Best For: Large hospitals, health systems, and multi-specialty provider groups that need enterprise-scale capabilities.
7. athenahealth
athenahealth is one of the most widely used practice management and billing platforms in the U.S., purpose-built for ambulatory and outpatient settings.
What sets it apart is the network effect—every payer rejection across its provider base feeds back into the rules engine, which means billing rules are constantly updated without manual intervention.
The platform combines EHR, billing, clearinghouse, and patient engagement into a single cloud suite.
Key Features:
- Network-powered rules engine learning from payer rejections in real time
- AI-powered insurance card scanning to reduce eligibility-related denials
- Enhanced Claim Resolution with SLA-backed denial management
- REST API endpoints and FHIR R4 support
- Marketplace of integrated third-party solutions
Best for: Physician practices, ambulatory groups, and mid-size health systems looking for an all-in-one outpatient EHR + billing platform.
8. Inovalon Provider Cloud
Inovalon provides a Provider Cloud suite with particular strength in Medicare-specific revenue cycle management.
The platform's core differentiator is its Insurance Discovery feature, which finds coverage for patients who reported no insurance—a major revenue recovery lever for Medicare-heavy organizations.
It also offers real-time FISS access, predictive cash flow forecasting, and denial trend analytics. If your payer mix skews heavily toward Medicare and you need analytics-driven RCM, Inovalon is built for that use case.
Key Features:
- Claims Management Medicare Pro with real-time FISS access and DDE verification
- Insurance Discovery for uninsured and underinsured patients
- Predictive cash flow forecasting and denial trend analytics
- Deep integration with PointClickCare and Epic
Best for: Medicare-heavy provider environments, large health systems, and long-term care facilities looking for analytics-driven revenue cycle optimization with strong insurance discovery capabilities.
9. SSI Group
SSI Group operates one of the largest institutional healthcare claims clearinghouses in the United States, with a significant share of U.S. hospitals relying on its infrastructure.
The platform is known for delivering one of the highest first-pass clean claim rates in the industry, powered by an extensive library of edit combinations across a broad payer network.
SSI integrates deeply with major EHR systems like Epic, Oracle Health (Cerner), and MEDITECH.
Key Features:
- Proprietary ClickON technology with extensive built-in edits
- Deep integrations with Epic, Oracle Health (Cerner), and MEDITECH
- ML-powered predictive payment analytics
- US-based support team with dedicated client relationships
Best for: Hospitals, health systems, long-term care, and skilled nursing organizations where first-pass acceptance rate improvements have direct, measurable revenue impact.
10. CollaborateMD
CollaborateMD is a cloud-based practice management and medical billing software with a built-in clearinghouse, designed for smaller billing operations.
The platform covers the essentials—scheduling, eligibility verification, claim submission, ERA auto-posting, patient billing, and reporting—all within a single cloud interface. Instead of AI or ML, CollaborateMD relies on rule-based automation to handle claim scrubbing and submission workflows.
For practices that want a proven, straightforward billing platform without enterprise pricing, CollaborateMD remains a solid choice.
Key Features:
- Built-in clearinghouse with Level 1 and Level 2 claim scrubbing
- Unlimited ERA with auto-posting
- Real-time eligibility verification
- Built-in reporting suite
Best For: Small-to-midsize practices and independent billing companies looking for affordable, cloud-based billing software that covers the fundamentals without unnecessary complexity.

How Hospitals Should Evaluate Medical Billing Platforms
Hospitals and healthcare organizations should evaluate medical billing platforms based on their ability to reduce denials, automate revenue cycle workflows, integrate with existing healthcare systems, and improve financial performance at scale.
While many billing tools offer similar core features, enterprise healthcare organizations need platforms that can handle high claim volumes, complex payer environments, multi-specialty operations, and strict compliance requirements.
The right medical billing solution is the one that closes the specific gaps costing your organization revenue integrity.
Below are the most common gaps organizations are trying to close and the capabilities to look for when evaluating a solution:
1. Denial Prevention and Claims Accuracy
One of the most important capabilities in a medical billing platform is proactive denial prevention.
Hospitals should evaluate whether the platform can:
- Identify coding and documentation issues before claim submission
- Detect payer-specific claim risks
- Automate claim scrubbing workflows
- Flag missing modifiers or authorization gaps
- Reduce manual rework for billing teams
2. AI and Workflow Automation
Modern healthcare billing platforms increasingly use AI to automate repetitive administrative tasks and improve operational efficiency.
Hospitals should assess:
- AI-assisted coding capabilities
- Automated charge capture workflows
- Intelligent work queues
- Predictive denial analytics
- Automated appeals management
- Payment posting automation
3. Payer-Specific Billing Logic
Generic HIPAA edits catch basic errors. Payer-specific rules catch the ones that actually cause denials. Strong medical billing solutions apply payer-specific SOPs, modifier rules, and billing guidelines before a claim is ever submitted.
4. EHR and System Integration
Medical billing software should integrate seamlessly with the hospital’s existing healthcare technology stack.
Key integrations include:
- Electronic Health Records (EHRs)
- Practice Management Systems (PMS)
- Clearinghouses
- Payer portals
- Patient billing systems
- Revenue cycle management tools
5. Human-in-the-Loop Design
AI should handle the routine; humans should handle the judgment calls. Understand exactly where the system hands off to your team—and whether that handoff is smooth or creates new bottlenecks.
Recommended reading: Common claim denial codes
6. Compliance
Your medical billing software should be HIPAA and SOC 2 certified, with a signed Business Associate Agreement (BAA) in place before any patient data flows into the system.
7. Vendor Support and Implementation Readiness
Implementation complexity can significantly impact billing transformation initiatives.
Hospitals should evaluate:
- Deployment timelines
- Training and onboarding support
- Dedicated account management
- Custom implementation services
- Migration support
- Ongoing optimization assistance
Automate Your Medical Billing End-to-End
The right AI medical billing solution should feel like adding a billing expert to your team—one that works around the clock, never misses a payer rule, and gets smarter with every claim.
Most billing tools solve one piece of the puzzle. CombineHealth's Mark solves the whole thing—from eligibility verification and charge entry to claim submission, payment posting, and denial prevention—in one autonomous, connected workflow.
If you're ready to move from manual billing to intelligent automation, book a demo with CombineHealth and see exactly how Mark fits into your revenue cycle.
FAQs
1. How is AI medical billing different from traditional billing software?
For large health systems, the best medical billing solutions combine deep payer connectivity, intelligent claim editing, and end-to-end automation. CombineHealth's Mark offers fully autonomous billing with human-in-the-loop oversight—ideal for high-volume organizations.
2. What are the main benefits of using AI for medical billing?
AI medical billing solutions reduce denial rates by catching errors pre-submission, accelerate payments by automating eligibility verification and payment posting, and eliminate the manual data entry that consumes billing staff time.
3. What is the best medical billing software for large health systems?
Traditional billing software helps staff submit claims faster but still requires manual intervention at most steps. AI-native medical billing solutions like CombineHealth's Mark make autonomous decisions—verifying eligibility, scrubbing claims, posting payments, following up on denials—without staff touching each step.
Recommended Reads
Related Posts
Lorem ipsum dolor sit amet, consectetur adipiscing elit. Suspendisse varius enim in eros elementum tristique. Duis cursus, mi quis viverra ornare, eros dolor interdum nulla, ut commodo diam libero vitae erat. Aenean faucibus nibh et justo cursus id rutrum lorem imperdiet. Nunc ut sem vitae risus tristique posuere.
Subscribe to newsletter - The RCM Pulse
Trusted by 200+ experts. Subscribe for curated AI and RCM insights delivered to your inbox
Let’s work together and help you get paid
Book a call with our experts and we'll show you exactly how our AI works and what ROI you can expect in your revenue cycle.
Email: info@combinehealth.ai

.webp)














