ER CPT Codes: Complete Guide to Emergency Department Coding
Learn ER CPT codes, E/M levels, procedures, and billing tips. A complete emergency department coding guide with examples, checklists, and workflow insights.
February 28, 2026


Key Takeaways:
• Describe both evaluation (E/M) services and procedures performed during emergency department visits, helping translate clinical care into standardized billing language.
• Emergency department E/M levels (99281–99285) are determined primarily by medical decision making, including problem complexity, data reviewed, and patient risk, not time spent.
• Common ER procedures include CPT codes for laceration repair, incision and drainage, fracture care, imaging interpretation, IV hydration, and critical care services.
• Accurate alignment between CPT codes and ICD-10 diagnoses is essential for demonstrating medical necessity and reducing denial risk.
• Frequent coding challenges include incorrect E/M leveling, incomplete procedure documentation, modifier errors, and CPT–ICD misalignment.
• A structured workflow, reviewing documentation, identifying procedures, validating MDM, and confirming payer rules, improves coding accuracy and first-pass claim acceptance.
• AI-assisted coding tools can enhance consistency by analyzing documentation, validating CPT–ICD alignment, and flagging issues before submission while keeping coders in control.
Emergency department coding differs significantly from medical coding in other care settings. These emergency department services involve rapid clinical evaluation, procedural interventions, and high-acuity decision making.
Patient acuity varies widely, documentation is created under pressure, and coding decisions depend heavily on medical decision making (MDM) rather than time spent with the patient. This makes selecting the right ER CPT codes both critical and challenging for medical coders and billers, while denial managers frequently review coding decisions to validate medical necessity and reduce claim risk.
Small errors, like choosing the wrong E/M level or missing supporting documentation, can easily lead to denials, compliance risks, or lost revenue. Additionally, as coding guidelines evolve and payer scrutiny increases, teams need clear frameworks to ensure accuracy.
This guide breaks down ER CPT codes into a practical reference, covering key code categories, E/M level selection, common pitfalls, and workflow best practices to help you code emergency department visits with confidence.
On this page
What Are ER CPT Codes?
ER CPT codes are standardized procedure and service codes used to describe the care delivered during an emergency department visit. These codes help translate clinical work into billable services so payers can understand:
- What was done
- Why was it medically necessary?
- How to calculate reimbursement
In emergency settings, CPT coding reflects both the evaluation performed and the procedures delivered, with medical decision-making guiding code selection.
Main Categories of ER CPT Codes
ER CPT codes generally fall into several categories that reflect the types of services performed during emergency department encounters:
- Evaluation and Management (E/M) codes,
- Procedure CPT codes
- Critical care codes
- ED independent interpretation codes
- Observation care codes
Understanding how these categories work together helps ensure accurate billing and reduces the risk of denials.
1. Emergency Department Evaluation and Management (E/M) Codes
E/M codes represent the provider’s evaluation of the patient and the complexity of clinical decision-making during the emergency encounter. These are the most commonly used ER CPT codes.
Incorrect E/M level selection can lead to undercoding when the documented complexity exceeds the code billed, or to overcoding when the selected level exceeds what the documentation supports, both of which may trigger audits or reimbursement issues.
ER Consult CPT Code
In the emergency department, consultation services are typically reported using the appropriate ER E/M code rather than separate consultation CPT codes. Many payers no longer recognize outpatient consultation codes (such as 99241–99245) in the ED setting.
Instead, providers report the ER E/M level (99281–99285) that reflects the complexity of the consultation work performed.
Before reporting consultation-related services, ensure:
- Payer policy allows consultation reporting in the ED
- A formal request for consultation is documented
- The provider’s findings and recommendations are clearly recorded
CPT Code for ER Follow-Up
Follow-up services in the emergency department are also reported under E/M coding, depending on the patient’s status and clinical work involved.
For instance,
- If a patient returns after discharge and requires a new evaluation, an appropriate ER E/M code (99281–99285) may apply based on documented MDM.
- If the patient remains under observation status, observation care codes such as 99218–99220 (initial observation care) or 99224–99226 (subsequent observation care) may be appropriate.
Documentation must clearly support:
- New or ongoing clinical decision-making
- Changes in patient condition
- Justification for additional evaluation
In addition to E/M services, emergency department encounters frequently involve procedural interventions that require separate CPT reporting.
2. Standard ER Procedure CPT Codes
Procedure CPT codes capture specific services performed during the visit. These are often billed alongside E/M codes when documentation supports separate work. During emergency department visits, procedures are frequently performed alongside evaluation services.
Common ER procedure CPT codes include:
These procedures may be billed in addition to E/M services when documentation shows they were performed as distinct, medically necessary services during the same visit.
Correctly distinguishing bundled services from separately billable procedures is a frequent challenge in ER coding.
3. Critical Care Codes
Critical care CPT codes are used when providers deliver intensive evaluation and management for patients with life-threatening conditions or a high risk of deterioration. These services involve continuous physician attention and complex clinical decision-making aimed at preventing organ failure, serious complications, or death.
The most commonly used emergency department critical care codes include:
Critical care coding is time-based but requires more than simply documenting duration. Providers must clearly demonstrate that:
- The patient’s condition was life-threatening or posed a significant risk
- Intensive monitoring or management was required
- Critical care activities were medically necessary and directly performed by the provider
Common examples include managing severe respiratory distress, septic shock, cardiac instability, or acute neurological emergencies.
4. ED Independent Interpretation Codes
ED independent interpretation CPT codes apply when emergency physicians personally review and interpret diagnostic tests rather than relying solely on external reports. These services may be separately billable when documentation confirms that the provider performed and documented their own clinical interpretation.
Independent interpretation is commonly used when emergency physicians analyze diagnostic data to guide immediate treatment decisions.
Common ED Independent Interpretation CPT Codes are:
To report independent interpretation services accurately:
- The physician’s interpretation must be documented in the medical record
- The interpretation must add clinical value beyond simply reviewing the report
- Payer-specific guidelines should be reviewed to confirm billing eligibility
Clear documentation ensures that the provider’s diagnostic work is appropriately recognized and reimbursed.
5. Observation Care Codes
Observation care CPT codes are used when patients require ongoing monitoring or evaluation but do not meet criteria for inpatient admission. Observation status allows clinicians to assess patient response to treatment, monitor evolving symptoms, or determine whether hospitalization is necessary.
Common observation care codes include:
Observation services often overlap with emergency department workflows, making clear documentation essential to distinguish observation care from standard ER E/M services.
How ER E/M Levels Are Determined
Under current guidelines, ER E/M code selection is primarily based on MDM rather than on time spent with the patient or on extensive documentation of history and exam components.
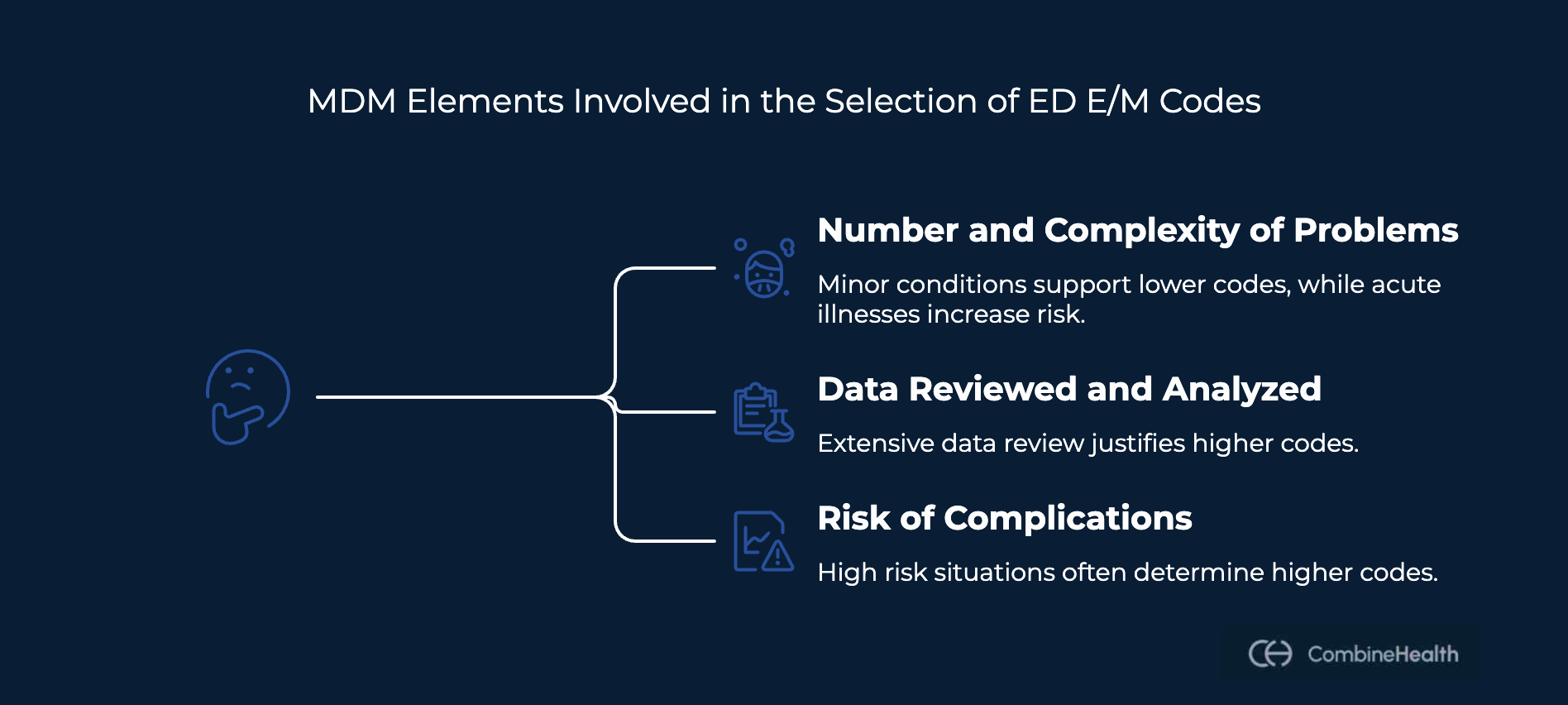
The three MDM elements involved in the selection of ED E/M codes are:
Number and Complexity of Problems Addressed
The first component of MDM evaluates the patient’s symptoms, conditions, or complaints that brought them to the emergency department and their clinical complexity. Minor or self-limited conditions typically support lower-level E/M codes, while acute illnesses, injuries requiring intervention, or unstable conditions increase the risk level. Documentation should clearly describe the severity of symptoms, differential diagnoses considered, and any escalation in clinical decision-making.
Data Reviewed and Analyzed
The second component involves the data reviewed or ordered during the emergency department visit. This may include laboratory tests, imaging studies, independent interpretation of results, or review of external medical records. Communication with other healthcare professionals or obtaining history from additional sources can also contribute to data complexity. Clear documentation of these activities helps justify higher-level E/M coding.
Risk of Complications and Management Decisions
Risk reflects both the patient’s condition and the provider's management decisions. Situations involving prescription drug management, decisions about hospitalization, or potential life-threatening complications generally indicate higher risk. In many cases, risk becomes the determining factor when choosing between moderate and high-level ER E/M codes.
Based on these MDM elements, the overall level of the visit is determined.
For instance, a minor issue such as evaluating an otherwise healthy child with a mild rash would typically reflect a straightforward or minimal MDM level, where CPT code 99281 may be appropriate.
Similarly, a patient presenting with severe chest pain, unstable vital signs, and suspected acute coronary syndrome would represent a high-complexity MDM level. In this scenario, the provider may order multiple diagnostic tests (such as ECG and cardiac enzymes), initiate urgent treatment, and consider hospital admission. The elevated risk, extensive data review, and complex management decisions would generally support a higher-level E/M code such as 99284 or 99285, depending on documentation and severity.
Accurate documentation of the problems addressed, diagnostic data reviewed, and risk involved is essential to ensure the selected CPT code aligns with the true complexity of the encounter.
Recommended Read: How to stay updated with the latest changes in medical coding guidelines
Common ER Medical Coding Mistakes That Lead to Denials
Emergency department coding errors often occur due to documentation gaps, fast-paced workflows, or unclear alignment between clinical care and coding guidelines. Here are some common ER medical coding mistakes seen in the emergency department:
Incorrect E/M Level Selection
One of the most common issues is selecting an E/M level based on perceived patient severity rather than documented MDM. Payers expect the complexity of the problem, the data reviewed, and the risk level to clearly support the chosen code. When documentation does not justify the level billed, claims are often downcoded or denied.
Incomplete Procedure Documentation
Emergency visits frequently involve procedures in addition to evaluation services. However, missing details such as technique, medical necessity, or provider involvement can lead to rejected procedure CPT codes. Coders must also be aware of bundling rules to avoid billing services that may already be included in another code.
CPT and ICD-10 Misalignment
Payers rely on diagnosis codes to validate medical necessity. When CPT codes do not align with ICD-10 diagnoses or the clinical narrative, claims may fail automated checks. Ensuring that procedures and services directly connect to documented patient conditions helps reduce denial risk.
Modifier Errors
Incorrect or missing modifiers can cause payers to interpret services as duplicate or not separately billable. Modifier misuse is a frequent source of rework, especially when procedures are performed during the same encounter as an E/M service.
Weak or Repetitive Documentation
Overuse of templated or copy-forward notes can weaken the clinical story behind the coding decision. Without clear evidence of provider reasoning or patient complexity, even correctly selected CPT codes may fail payer review.
Step-by-Step ER Coding Workflow
Emergency department coding works best when it follows a structured review process. Because ER visits involve multiple variables, such as patient acuity, procedures, diagnostic data, and payer rules, a structured process ensures that emergency department services are accurately captured and supported by documentation.
Below is a simplified framework that many high-performing revenue cycle teams follow.
Step 1: Review Provider Documentation
The workflow begins with a careful review of provider-authored notes. Coders evaluate the patient’s presenting symptoms, clinical findings, differential diagnoses, and treatment plan. The goal is to understand the full scope of care delivered during the encounter. Each of these emergency department visits must be reviewed individually to ensure accurate code assignment.
Clear documentation of MDM is critical at this stage, as it directly impacts E/M level selection.
Step 2: Identify Billable Procedures
Next, coders determine whether any separately reportable procedures were performed. This may include laceration repairs, fracture management, imaging interpretation, IV therapy, or critical care services.
Each procedure must be fully documented and medically necessary. Coders also confirm whether bundling rules apply before assigning additional CPT codes.
Step 3: Determine the Correct E/M Level
Coders confirm the E/M level based on documented MDM. The selected code must clearly align with the provider’s documented clinical reasoning.
This step is where many ER coding discrepancies occur, making careful review essential.
Step 4: Assign and Sequence ICD-10 Codes
After CPT codes are identified, diagnosis codes must accurately reflect the patient’s condition and support medical necessity. Proper sequencing ensures that payers can clearly see the clinical justification behind billed services.
Misalignment between CPT and ICD-10 codes is a common source of denials, so this validation step is critical.
Step 5: Validate Payer-Specific Rules
Before submission, teams should verify payer requirements, modifier usage, and policy updates that may affect reimbursement. Differences in payer interpretation can impact how ER CPT codes are reviewed and processed.
How CombineHealth’s Amy Supports ER Coding Workflows
In high-volume emergency settings, maintaining this level of review consistency can be difficult. This is where structured AI support can enhance accuracy without replacing human oversight.
CombineHealth’s Amy, an AI Medical Coding Solution, evaluates provider-authored notes, procedures performed, tests ordered, and facility resource usage to identify appropriate CPT codes. Once CPT codes are generated, Amy moves to ICD-10 coding, analyzing presenting symptoms, acute issues, and chronic conditions that impact complexity.
After generating diagnosis codes, Amy performs a second validation pass. She confirms that each CPT code is clinically justified by the selected ICD codes. If misalignment is detected, the system either retries the mapping logic or flags the case for human review.
This human-in-the-loop approach mirrors how experienced coders think, reviewing documentation, validating medical necessity, and confirming alignment, while improving speed and consistency across high-volume ER workflows.
Building a More Accurate and Efficient ER Coding Process
In ER CPT coding, a structured workflow makes the difference. When teams consistently review documentation, determine E/M levels based on medical decision making, validate procedure support, and confirm CPT–ICD alignment before submission, coding becomes more accurate and defensible.
AI-assisted validation can further strengthen this process. AI medical coding solutions that analyze provider notes, suggest appropriate ER CPT codes, generate supporting ICD-10 codes, and flag misalignment before claims are submitted help reduce rework and improve first-pass yield, while keeping coders in control.
If your emergency department is struggling with denials, coding variability, or manual review overload, it may be time to rethink your workflow. See how CombineHealth’s AI coding agents support ER CPT code accuracy in real workflows — book a demo to explore how your team can reduce denials and improve coding consistency without increasing administrative burden.
FAQ
1. What are ER CPT codes?
ER CPT codes are standardized billing codes used to report services and procedures performed during an emergency department visit. They include E/M codes for evaluation and procedure codes for specific treatments.
2. What is the CPT code for an ER visit?
The most common CPT codes for emergency room visits are 99281–99285. The correct code depends on the level of medical decision-making, patient complexity, and clinical risk documented during the encounter.
3. How are ER E/M levels determined?
ER E/M levels are determined based on medical decision making, which includes the number and complexity of problems addressed, the data reviewed, and the risk of complications or management decisions. Selecting the correct CPT code for an ER visit requires clear documentation of MDM complexity and associated risk.
4. Can ER procedure CPT codes be billed with E/M codes?
Yes, procedure CPT codes can be billed in addition to E/M codes if documentation clearly supports separate and medically necessary services. Proper modifier use may also be required.
5. Why do ER claims get denied?
Common reasons include incorrect E/M level selection, CPT–ICD misalignment, missing procedure documentation, and modifier errors. A structured validation process before submission can significantly reduce denial risk.
Recommended Reads
Related Posts
Lorem ipsum dolor sit amet, consectetur adipiscing elit. Suspendisse varius enim in eros elementum tristique. Duis cursus, mi quis viverra ornare, eros dolor interdum nulla, ut commodo diam libero vitae erat. Aenean faucibus nibh et justo cursus id rutrum lorem imperdiet. Nunc ut sem vitae risus tristique posuere.
Subscribe to newsletter - The RCM Pulse
Trusted by 200+ experts. Subscribe for curated AI and RCM insights delivered to your inbox
Let’s work together and help you get paid
Book a call with our experts and we'll show you exactly how our AI works and what ROI you can expect in your revenue cycle.
Email: info@combinehealth.ai


.webp)













