Revenue Cycle Management Challenges in Healthcare and How To Overcome Them
Explore key RCM challenges in healthcare, from rising denials to staffing gaps and prior auth delays, and how leaders are solving them in 2026.
March 30, 2026


Key Takeaways:
• In 2025, hospitals spent $43 billion trying to collect payments insurers already owed, a figure that reflects the full administrative cost of a revenue cycle under pressure from every direction.
• Payer complexity, prior authorization bottlenecks, coding errors, staffing shortages, A/R delays, and fragmented systems are the six challenges draining the most revenue from healthcare organizations in 2026.
• Most RCM challenges follow predictable patterns, which means they respond to structured fixes: moving denial prevention upstream, building payer intelligence into workflows, and prioritizing A/R by recovery probability are where the highest-impact gains happen.
• 85% of healthcare leaders are already exploring or adopting generative AI, making AI-powered RCM a competitive advantage.
Every payer runs by its own rules—different documentation requirements, different prior authorization protocols, different billing edits. For RCM teams already stretched thin, that complexity doesn’t stay manageable for long. These hospital revenue cycle management challenges continue to evolve.
The cracks show up in the data itself. 60% of medical group leaders reported an increase in claim denial rates in 2024 compared to the prior year, per an MGMA Stat poll.
Behind that number is a billing team spending hours on rework, appeals, and resubmissions for claims that should have been paid the first time.
Understanding where these breakdowns happen (and why) is the first step toward fixing them.
This article covers the most pressing revenue cycle management challenges in healthcare, what each costs, and what RCM leaders are doing today to overcome these challenges.
On this page
Common Revenue Cycle Management Challenges in 2026

Here’s what that RCM complexity looks like in practice and where it’s hitting revenue cycle teams hardest:
1. Payer Complexity and Rising Administrative Burden
Getting paid for care already delivered has never been this complicated.
Payers have steadily tightened the claims review process, applied stricter medical necessity criteria, and expanded documentation requirements post-submission.
For revenue cycle teams, this creates a moving target—one that shifts with every payer update and every new coverage policy.
In 2025 alone, hospitals spent $43 billion in total, trying to collect payments insurers already owed for care delivered, according to the American Hospital Association.
That figure captures the full administrative cost of what payer complexity produces—denied claims, rework cycles, appeals, and staff hours consumed chasing reimbursement on every front.
The gap between what providers bill and what they collect widens with each layer of complexity added. Payer complexity is entirely outside the organization's control and can only be solved with the right workflows in place. This remains one of the most persistent hospital RCM challenges across organizations.
2. Prior Authorization Delays
Prior authorization sits at the front end of the revenue cycle, which means when it fails, everything downstream fails with it.
A missed or expired authorization stops revenue before it starts by:
- delaying procedures
- disrupting scheduling
- pushing the entire reimbursement timeline back
The damage compounds before a single claim is even submitted.
The American Medical Association’s 2024 survey found that the average practice completes 39 prior authorization requests per week, consuming 13 hours of staff time. That’s nearly two full workdays spent on the prior authorization admin process alone.
Unlike coding errors, prior-authorization-related denials often can't be corrected and resubmitted. They require a full appeal cycle to recover. And every day spent in that appeal cycle is a day the revenue sits uncollected.
Recommended reading: How to Appeal an Insurance Claim Denial
3. Coding Inaccuracy Due to Clinical Documentation Gaps
Coding errors are one of the most common reasons for claim denials.
Errors such as a mismatched diagnosis to procedure code, a missing modifier, or an incorrect billing sequence can trigger a rejection that sends the claim back to the billing team for correction. And often, the root cause leads back to documentation errors on the providers’ end.
That back-and-forth between billers and providers to gather missing documentation or clarify clinical details can add days to the reimbursement cycle and pull both teams away from higher-value work.
This is a system-wide problem with a measurable financial cost. CMS's FY2025 improper payments report puts Medicare FFS improper payments at $28.83 billion—citing insufficient provider documentation as the primary driver.
Every rejected claim that circles back for correction is time spent recovering revenue that should have been collected on first submission.
4. Staffing Shortages and a High Cost of Losing Institutional Knowledge
Staffing gaps continue to be one of the most critical hospital revenue cycle management challenges impacting operational efficiency.
RCM departments have been operating under sustained workforce pressure for years.
Positions stay vacant for months, workloads fall on whoever remains, and the cycle of hiring, training, and losing staff has become a recurring cycle for most billing teams.
This isn’t anecdotal. 56% of medical groups reported their days in A/R increased because of staffing difficulties, per the MGMA poll.
Each departure takes payer-specific knowledge that took years to accumulate and cannot be transferred in a 90-day onboarding cycle. The replacement produces more errors, generates more denials, and creates more rework.
That knowledge gap is where staffing shortages do their quietest damage. Lost institutional knowledge isn't fully visible until it shows up in rising denial rates and falling clean claim ratios.

5. Claim Filing Delays and A/R Follow-Up Gaps
Every payer sets a strict deadline for submission.
If the team misses it, the claim becomes a hard denial with no appeal pathway or recovery. For billing teams managing high claim volumes across multiple payers, each with different timelines and filing requirements, staying ahead of those deadlines is a constant risk.
When claims stack up in follow-up queues, the financial exposure compounds quietly—as many as 60% of denied claims are never resubmitted, according to AHIMA. That’s revenue that simply ran out of bandwidth to pursue.
The further a claim ages, the harder it becomes to collect. With every passing week, appeal windows close, documentation becomes harder to retrieve, and payer follow-up grows more complex.
By the time an aging claim gets worked, the path to full recovery is rarely straightforward.
Recommended reading: Common AR Scenarios in Healthcare
6. Workflow Inefficiencies and Outdated Systems
Fragmented systems turn every hospital revenue cycle management challenge harder to manage.
When EHRs, practice management platforms, clearinghouses, and payer portals don't communicate cleanly, billing staff spend significant time manually reconciling data across disconnected systems rather than processing claims.
That manual effort introduces new kinds of transcription errors that trigger clearinghouse rejections and payer-level denials.
Layering a new technology or a solution on top of a fragmented workflow is rarely a fix. The underlying problem is the interoperability gaps between systems, not the systems themselves.
How to Navigate Revenue Cycle Management Challenges
The steps below are some of the highest-impact plays in the RCM leader's playbook today:
1. Move Denial Prevention Upstream
Most denials trace back to front-end failures—missing authorizations, eligibility gaps, and documentation that doesn’t support the billed service.
Fixing these at the point of encounter is exponentially cheaper than fixing them post-denial. Front-end claim scrubbing, real-time eligibility verification, and authorization checks initiated at the point of ordering are where the highest-impact prevention happens.
2. Standardize Workflows Across the Revenue Cycle
Inconsistent processes create inconsistent outcomes.
When every team member, location, and service line follows the same submission protocols, the same documentation standards, and the same denial response workflows, errors become easier to spot and faster to fix.
3. Run Coding Audits and Close the Feedback Loop
Denial patterns repeat when root causes go unaddressed.
Regular medical coding audits of claims—by payer, by provider, by denial type—surface the specific errors driving rejections. Feeding those findings back into coder training and workflow updates is what stops the same denials from cycling through month after month.
4. Prioritize A/R by Recovery Probability
Not every single claim deserves equal attention.
Triaging the A/R pipeline by financial value, payer, denial type, and appeal deadlines (rather than working chronologically) recovers more revenue with the same bandwidth you have. The goal is to make sure the highest-value, most recoverable claims get worked first before appeal windows close.
5. Build Payer Intelligence Into Your Workflows
Every payer has different document thresholds, different denial patterns, and different appeals overturn rates.
Organizations that track these payer-specific denial trends and adjust their submission protocols accordingly can stop making the same mistakes twice. Regular audits of payer behavior are what separate teams that prevent denials from teams that just recover them.
6. Improve Visibility Across Revenue Cycle
Real-time dashboards that aggregate data across payers, service lines, and locations give RCM leaders the ability to act on problems before they compound.
Denial trends, A/R aging, and clean claim rates should be visible in real time and not surfacing weeks later in a monthly report when the damage is already done.
Recommended reading: An Expert-Backed Playbook for Managing Claim Denials
Why Optimizing Your Healthcare Revenue Matters
A well-optimized revenue cycle can lead to cleaner claims, faster reimbursements, and fewer write-offs. It gives finance teams the cash flow predictability they need to make smarter operational decisions. It also reduces the admin workload from the billing staff.
Beyond financials and efficiency, RCM optimization directly affects organizational resilience over time. Teams that catch denial patterns early, manage A/R proactively, and stay on top of payer policy changes operate from a position of control.
That's the difference between a revenue cycle that sustains the organization and one that quietly drains it.
How AI Helps Overcome these RCM Challenges
The playbook above outlines what needs to happen across the revenue cycle.
But the harder question we need to ask is capacity—who executes it, and when, alongside everything else that is already on the plate.
Here’s where AI can change the equation. It doesn’t aim to replace experienced professionals but rather help them by absorbing high-volume, rule-intensive work that consumes their valuable time.
This frees them to focus on the exceptions, edge cases, and the strategic decisions that actually move the needle.
The industry is already moving in this direction. According to a McKinsey survey, 85% of healthcare leaders are already exploring or adopting generative AI, and among those implementing it, 64% report positive ROI. The organizations seeing results are embedding AI into the core of their revenue cycle operations.
CombineHealth is one such platform—an integrated AI workforce built specifically for healthcare RCM, where each agent handles a distinct function across the full revenue cycle and communicates with the others to continuously improve outcomes.
CombineHealth’s AI Agents for Every Stage of Revenue Cycle
- Jessica (AI Medical Scribe Solution) captures patient encounters in real time and auto-structures notes for coding and billing accuracy. She flags missing details before the encounter closes, so documentation gaps don't make it into the coding workflow.
- Amy (AI Medical Coding Solution) reads encounter notes directly from the EMR and assigns codes with 99.2%+ accuracy—identifying undercoding and overcoding in real time. Every decision comes with a line-by-line rationale, and complex cases get flagged for human review.
- Mark (AI Medical Billing Solution) automates claim generation, performs real-time eligibility verification across 50+ payer portals, and submits clean claims through clearinghouses. He reads ERAs and EOBs, posts payments, and learns continuously from prior denial patterns.
- Penny (AI Policy Review Solution) validates claims against Medicare, Medicaid, and commercial payer guidelines before submission—flagging policy mismatches and generating risk scores for at-risk claims.
- Adam (AI Denial Management Solution) categorizes denials by root cause, makes AI-driven calls to payers, and prioritizes cases by age, dollar value, and payer. He builds payer scorecards and uses predictive analytics to prevent recurring denial patterns before they compound.
- Rachel (AI Medical Appeals Solution) drafts evidence-based appeals using clinical documentation extracted directly from provider notes—adapting to your organization's writing style. She predicts appeal success probability and monitors filing deadlines across all open cases.
- Taylor (AI Revenue Cycle Analytics Solutions) monitors A/R aging, first-pass acceptance, and cash flow in real time—flagging revenue leakage before it hits the bottom line. She feeds insights back upstream to Amy, Mark, and Adam, making data actionable across the full cycle.
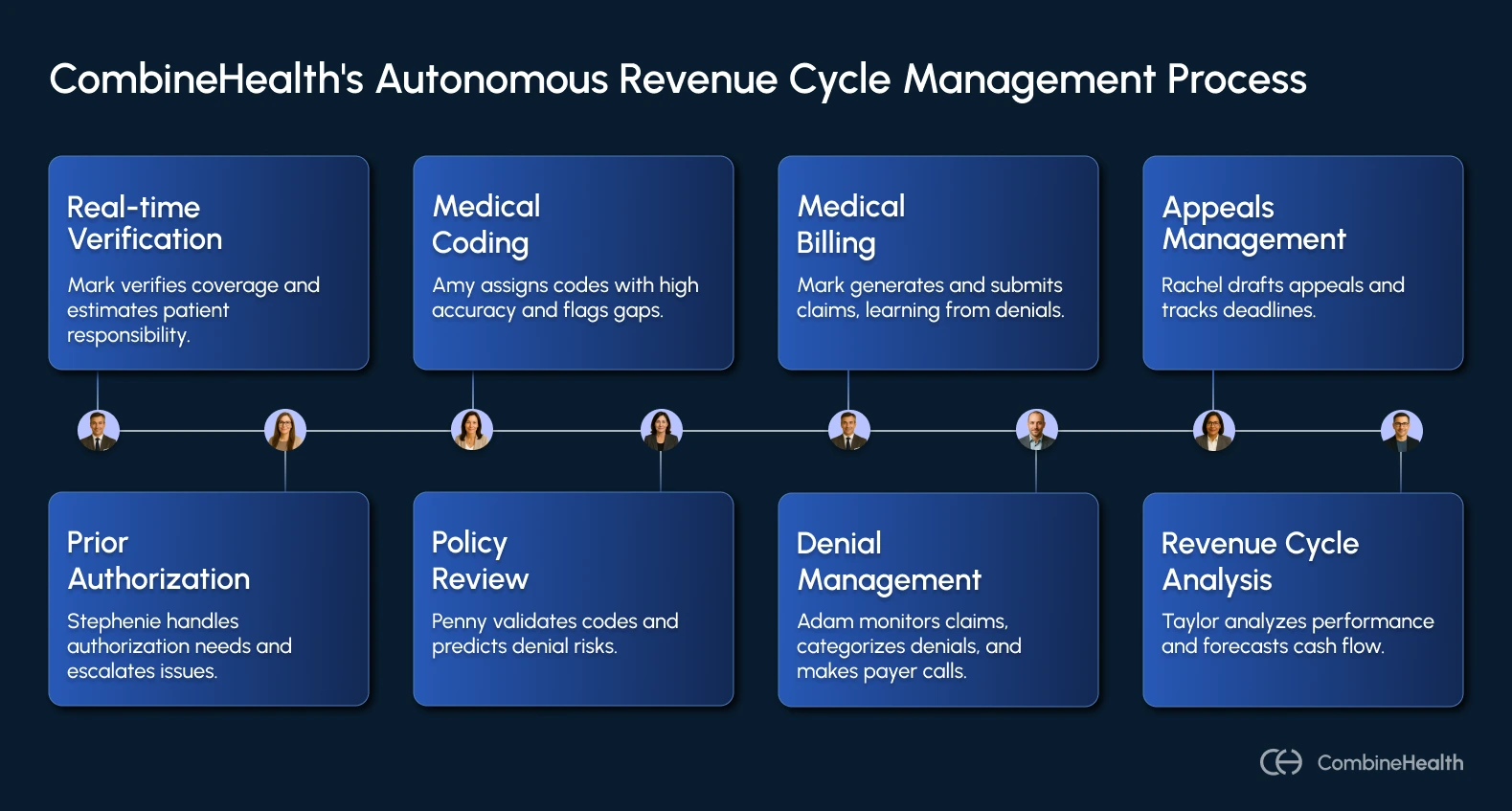
These end-to-end AI agents work independently across their respective functions and communicate with one another when needed to ensure every stage of your revenue cycle is covered.
Take Control of Your Health System’s Revenue!
Revenue cycle management challenges in healthcare aren't going away. Denial rates will keep climbing, payer requirements will keep tightening, and staffing pressures will keep demanding more from your teams.
The organizations building financial resilience in 2026 are the ones replacing reactive workflows with proactive, AI-powered systems—catching problems before they become denials, resolving denials before they become write-offs, and running their revenue cycles with the visibility that lets them act on data rather than catch up to it.
Book a demo to see how CombineHealth's AI agents work across your revenue cycle and what that looks like for your denial rates, A/R days, and collections!
FAQs
1. What are the most common revenue cycle management challenges in healthcare?
The most common RCM challenges include payer complexity and rising administrative burden, prior authorization delays, coding accuracy and documentation gaps, staffing shortages, claim filing delays, and workflow inefficiencies.
2. How do rising claim denials impact hospital revenue cycle management?
Denied claims reduce cash flow, increase days in A/R, and consume staff bandwidth in rework and appeals. In 2025, hospitals spent $43 billion trying to collect payments insurers already owed. A figure that reflects the full administrative cost of managing denials at scale.
3. How do prior authorization delays affect the revenue cycle?
When prior authorization fails, everything downstream is affected. Missed or expired authorizations generate outright claim denials, delay procedures, and push the entire reimbursement timeline back.
4. How does AI help overcome revenue cycle management challenges?
AI helps automate the high-volume, rule-intensive tasks where manual errors are most common, such as coding, claim scrubbing, eligibility verification, denial categorization, and payer follow-up. This reduces denial rates, accelerates cash through the cycle, and frees experienced staff for the complex cases that require human judgment.
Recommended Reads
Related Posts
Lorem ipsum dolor sit amet, consectetur adipiscing elit. Suspendisse varius enim in eros elementum tristique. Duis cursus, mi quis viverra ornare, eros dolor interdum nulla, ut commodo diam libero vitae erat. Aenean faucibus nibh et justo cursus id rutrum lorem imperdiet. Nunc ut sem vitae risus tristique posuere.
Subscribe to newsletter - The RCM Pulse
Trusted by 200+ experts. Subscribe for curated AI and RCM insights delivered to your inbox
Let’s work together and help you get paid
Book a call with our experts and we'll show you exactly how our AI works and what ROI you can expect in your revenue cycle.
Email: info@combinehealth.ai
















